
Chronic health conditions have become one of the greatest medical challenges of our time. Conditions such as autoimmune disease, metabolic syndrome, diabetes, cardiovascular disease, neurodegenerative disorders, and even many cancers are rising at unprecedented rates. While conventional medicine often focuses on managing symptoms, many practitioners and patients are beginning to recognize the need for a deeper, more personalized approach.
A metabolic approach to health focuses on addressing the underlying biological processes that influence disease development. Instead of treating symptoms in isolation, this approach considers how metabolism, genetics, immune function, environmental exposures, and lifestyle factors interact to shape long-term health outcomes.
By addressing these interconnected systems, an individualized metabolic strategy can help support the body’s natural ability to restore balance and resilience.
This model emphasizes personalized medicine, lifestyle medicine, and functional health principles to support long-term healing and disease prevention.
A metabolic approach to health is a systems-based framework that focuses on optimizing the body’s metabolic processes to support overall health and resilience.
Metabolism refers to the complex network of biochemical reactions that sustain life. These reactions regulate energy production, cellular repair, hormone signaling, immune defense, detoxification, and inflammation control.
When metabolic processes become dysregulated due to poor nutrition, chronic stress, environmental toxins, disrupted circadian rhythms, or genetic vulnerabilities, chronic disease can develop.
Rather than targeting a single symptom or organ system, a metabolic health model addresses the root drivers of dysfunction across multiple physiological systems.
Key goals of a metabolic health strategy include:
• Supporting cellular energy production
• Reducing chronic inflammation
• Stabilizing blood sugar and insulin signaling
• Optimizing immune system function
• Restoring hormonal balance
• Supporting detoxification pathways
• Improving mental and emotional resilience
When these systems function efficiently, the body becomes more capable of maintaining long-term health.
Every individual has a unique biological makeup. Genetics, lifestyle choices, environmental exposures, gut microbiome composition, and stress levels all influence how disease develops.
This means that two individuals with the same diagnosis may require completely different interventions.
For example:
One person with autoimmune disease may primarily struggle with gut microbiome imbalance and chronic inflammation.
Another may be dealing with toxin exposure, hormonal dysregulation, and circadian rhythm disruption.
An individualized metabolic strategy evaluates each person’s unique biological terrain, allowing practitioners to identify the underlying factors contributing to chronic health challenges.
By addressing these root causes, treatment can move beyond symptom management toward long-term restoration of health.
While genetics influence disease risk, genes are not destiny. Epigenetics refers to how lifestyle and environmental factors regulate gene expression.
Diet, physical activity, sleep quality, toxin exposure, and stress levels can all activate or silence specific genes.
Nutritional epigenetics has shown that nutrients such as polyphenols, omega-3 fatty acids, and certain plant compounds can influence pathways involved in inflammation, detoxification, and cellular repair.
By optimizing lifestyle factors, individuals can support beneficial gene expression patterns that promote health.
Blood sugar regulation plays a central role in metabolic health.
Chronically elevated blood glucose and insulin levels contribute to:
• Inflammation
• Hormonal imbalance
• Cardiovascular disease
• Cognitive decline
• Weight gain
• Increased cancer risk
Stabilizing blood sugar through nutrient-dense foods, balanced macronutrients, physical activity, and intermittent fasting strategies can significantly improve metabolic efficiency.
Modern environments expose individuals to thousands of chemicals through food, air, water, and consumer products.
These toxins can disrupt endocrine function, impair detoxification pathways, damage mitochondria, and increase oxidative stress.
A metabolic health approach evaluates toxic exposures and supports detoxification pathways through:
• Nutrient support
• Gut health optimization
• Liver function support
• Lifestyle strategies that reduce exposure
Reducing toxic burden allows the body’s metabolic systems to function more efficiently.
The gut microbiome plays a crucial role in metabolism, immune regulation, neurotransmitter production, and inflammation control.
Microbial imbalances can contribute to:
• Autoimmune disease
• Mood disorders
• Digestive dysfunction
• Insulin resistance
• Chronic inflammation
Strategies to restore microbial diversity may include dietary fiber, fermented foods, targeted probiotics, and reduction of inflammatory dietary triggers.
A healthy microbiome supports both metabolic health and immune resilience.
The immune system must maintain a delicate balance between defense and tolerance.
When immune function becomes dysregulated, chronic inflammation and autoimmune disease can develop.
A metabolic approach supports immune efficiency through:
• Gut health restoration
• Nutritional sufficiency
• Stress regulation
• Adequate sleep
• Anti-inflammatory dietary patterns
Optimizing immune function helps the body respond appropriately to threats without creating excessive inflammatory damage.
Chronic inflammation is a common underlying factor in many diseases.
Conditions such as cardiovascular disease, diabetes, Alzheimer’s disease, arthritis, and metabolic syndrome are all associated with persistent inflammatory signaling.
Reducing inflammation involves:
• Anti-inflammatory nutrition
• Optimizing omega-3 fatty acid intake
• Supporting antioxidant defenses
• Managing stress
• Improving sleep quality
Addressing oxidative stress at the cellular level can significantly improve long-term metabolic health.
Healthy circulation ensures that tissues receive adequate oxygen and nutrients.
At the same time, certain disease processes—including cancer—can involve excessive angiogenesis, or abnormal blood vessel formation.
Metabolic health strategies may focus on:
• Improving vascular health
• Supporting nitric oxide pathways
• Promoting healthy blood flow
• Incorporating anti-angiogenic foods rich in polyphenols and phytonutrients
These strategies support overall cardiovascular and cellular health.
Hormones regulate nearly every physiological process in the body.
Imbalances in insulin, cortisol, thyroid hormones, estrogen, progesterone, and testosterone can disrupt metabolic function.
Lifestyle factors strongly influence hormonal health.
These include:
• Sleep patterns
• Stress levels
• Nutritional intake
• Body composition
• Environmental toxin exposure
A metabolic health framework seeks to restore hormonal equilibrium through lifestyle and targeted therapeutic interventions.
Chronic stress is one of the most powerful disruptors of metabolic health.
Elevated cortisol levels can impair immune function, increase inflammation, disrupt sleep, and worsen insulin resistance.
Equally important are circadian rhythms—the natural biological cycles that regulate sleep, hormone release, and metabolism.
Supporting healthy circadian rhythms through consistent sleep schedules, sunlight exposure, stress management practices, and mindful lifestyle habits can dramatically improve metabolic function.
Mental and emotional health are inseparable from physical health.
Chronic stress, trauma, anxiety, and depression can all influence metabolic pathways, immune signaling, and inflammation levels.
A holistic metabolic health strategy includes practices that support emotional resilience such as:
• Mindfulness
• Meditation
• Breathwork
• Social connection
• Purposeful living
When emotional health improves, physiological healing often follows.
Healthcare is gradually shifting from reactive disease management toward preventive, personalized medicine.
A metabolic approach to health recognizes that chronic diseases arise from complex interactions between genetics, environment, lifestyle, and metabolic processes.
By addressing these interconnected systems simultaneously, practitioners can support long-term healing rather than simply suppressing symptoms.
This model empowers individuals to actively participate in their health through lifestyle adjustments, targeted nutrition, stress management, and environmental awareness.
Ultimately, metabolic health represents a powerful framework for improving both longevity and quality of life.
A metabolic approach to health is a systems-based strategy that focuses on optimizing the body’s metabolic processes to improve overall wellness and address chronic disease. Rather than treating individual symptoms, this approach looks at how factors such as nutrition, blood sugar regulation, inflammation, gut health, hormone balance, environmental toxins, and stress influence the body’s cellular metabolism. By improving these underlying processes, the body can better restore balance and support long-term health.
Metabolism regulates how the body produces energy, repairs cells, balances hormones, and manages inflammation. When metabolic processes become disrupted—due to poor diet, stress, toxins, or lifestyle factors—the body can develop chronic inflammation, insulin resistance, hormonal imbalances, and immune dysfunction. These metabolic disruptions are linked to many chronic conditions including diabetes, cardiovascular disease, autoimmune disorders, neurodegenerative diseases, and metabolic syndrome.
A metabolic approach may support individuals dealing with a wide range of chronic health conditions, including:
• Metabolic syndrome
• Type 2 diabetes
• Autoimmune diseases
• Chronic fatigue
• Hormonal imbalance
• Digestive disorders
• Cardiovascular disease
• Neurodegenerative conditions
• Chronic inflammation
Because it focuses on underlying biological systems, metabolic health strategies can be adapted to many different conditions.
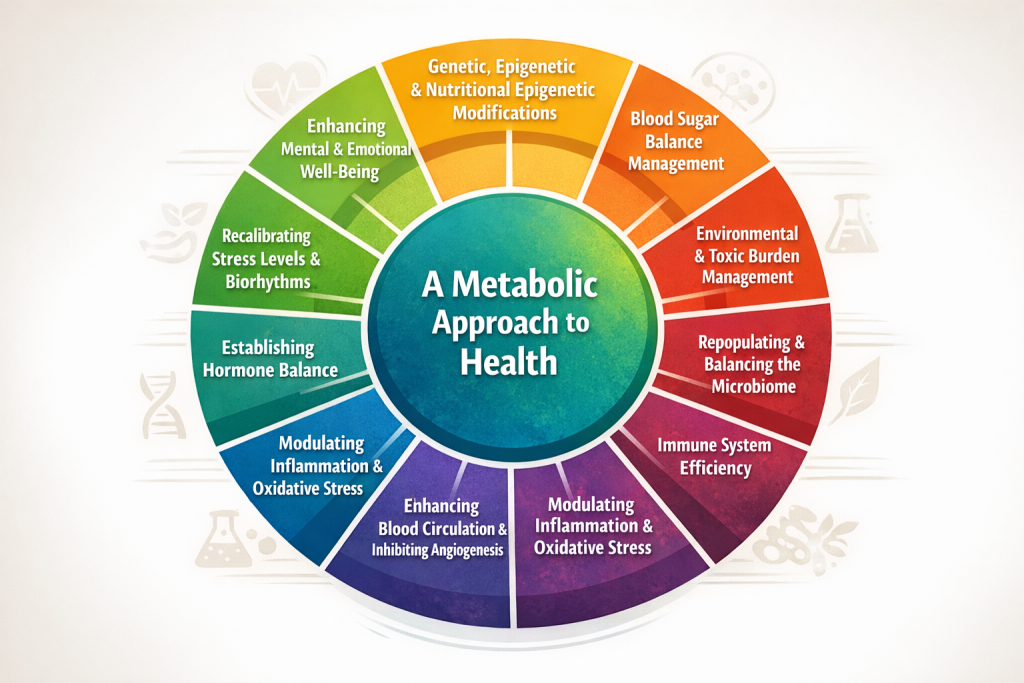
A metabolic approach to health focuses on several interconnected systems that influence wellness. These commonly include:
Genetic and epigenetic regulation through lifestyle
Blood sugar balance and metabolic stability
Environmental toxin reduction
Gut microbiome balance
Immune system efficiency
Inflammation and oxidative stress control
Healthy circulation and vascular support
Hormone balance
Stress management and circadian rhythm regulation
Mental and emotional well-being
These pillars work together to support the body’s natural healing processes.
Blood sugar regulation plays a central role in metabolic health. Frequent spikes in glucose and insulin can increase inflammation, disrupt hormone signaling, damage blood vessels, and promote weight gain. Over time, unstable blood sugar can contribute to insulin resistance and metabolic syndrome. Supporting stable blood sugar through balanced nutrition, regular movement, and healthy sleep patterns can significantly improve metabolic function.
The gut microbiome influences many metabolic processes including digestion, immune function, inflammation regulation, and even mood. Beneficial gut bacteria help break down nutrients, produce important metabolites, and support immune tolerance. When the microbiome becomes imbalanced, it can contribute to inflammation, insulin resistance, and digestive disorders. Supporting gut health through fiber-rich foods, fermented foods, and diverse nutrition helps maintain metabolic balance.
Yes. This concept is known as epigenetics, which refers to how environmental and lifestyle factors influence gene activity. While your DNA sequence remains the same, lifestyle choices such as diet, physical activity, stress management, and sleep can turn certain genes on or off. These epigenetic changes can influence inflammation, detoxification pathways, metabolism, and disease risk.
Environmental toxins can interfere with hormone signaling, damage mitochondria, disrupt detoxification pathways, and increase oxidative stress. These effects can impair metabolism and contribute to chronic disease. Reducing exposure to toxins in food, water, air, and consumer products helps support the body’s natural detoxification systems and metabolic efficiency.
Chronic stress elevates cortisol levels, which can disrupt blood sugar regulation, impair immune function, increase inflammation, and disturb sleep patterns. Over time, persistent stress can lead to metabolic dysfunction and hormonal imbalance. Practices such as mindfulness, breathing exercises, adequate sleep, and regular movement can help regulate the stress response and improve metabolic resilience.
A metabolic approach to health overlaps with principles used in functional and integrative medicine. All of these approaches focus on identifying root causes of disease rather than simply managing symptoms. They also emphasize personalized care, lifestyle medicine, nutrition, and systems biology to support long-term wellness.
Every individual has a unique metabolic profile influenced by genetics, lifestyle habits, environmental exposures, gut microbiome composition, and stress levels. Personalized metabolic health plans evaluate these factors through health history, lifestyle assessment, and sometimes laboratory testing. Based on this information, targeted strategies can be developed to support the systems most in need of balance.
Simple lifestyle habits can begin improving metabolic health, including:
• Eating whole, nutrient-dense foods
• Balancing protein, healthy fats, and fiber at meals
• Getting consistent, restorative sleep
• Reducing ultra-processed foods and sugar intake
• Moving the body regularly
• Managing stress through mindfulness or relaxation techniques
• Supporting gut health through dietary diversity
Small daily improvements can have powerful effects on long-term metabolic function.
Improvements in metabolic health can begin within weeks of consistent lifestyle changes, especially when focusing on nutrition, sleep, and blood sugar stability. However, deeper metabolic restoration often occurs gradually over several months as inflammation decreases, hormone balance improves, and cellular processes become more efficient.
Chronic illness rarely results from a single cause. Instead, it typically arises from multiple interacting factors such as inflammation, nutrient deficiencies, toxin exposure, gut imbalance, and stress. A systems-based metabolic approach recognizes these connections and addresses the underlying biological networks involved in health and disease.