]
[/caption]

Cortisol and adrenal fatigue symptoms have become some of the most talked-about hormones in modern health—and for good reason. As the body’s primary stress hormone, it plays a central role in energy, metabolism, immune function, and our ability to respond to daily demands.
At the same time, more people are struggling with persistent symptoms like fatigue, poor sleep, brain fog, and burnout. Many have sought answers through conventional medical care, only to be told that their lab work is “normal,” leaving them without clear direction or support.
This gap has led to growing interest in terms like adrenal burnout or adrenal fatigue. While these terms are not formally recognized in conventional endocrinology, they often reflect a very real experience: the body’s reduced ability to adapt to chronic stress.
From an integrative medicine perspective, the goal is not simply to label a condition—but to understand why the body is struggling in the first place.
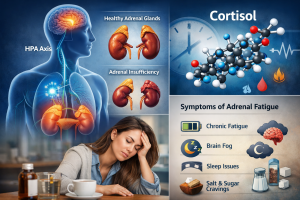
Cortisol is a hormone produced by the adrenal glands that helps regulate:
Stress response
Blood sugar levels
Inflammation
Blood pressure
Sleep-wake cycles
It follows a natural rhythm—higher in the morning and lower at night. When this rhythm becomes disrupted, it can lead to symptoms such as fatigue, anxiety, poor sleep, and metabolic imbalance.
Adrenal burnout (often called adrenal fatigue symptoms) is a non-medical term used to describe a group of symptoms such as fatigue, sleep disturbances, brain fog, and cravings that are associated with chronic stress and dysregulation of the body’s stress response system.
The term “adrenal burnout” is widely used in integrative and functional medicine, but it is not recognized as a formal medical diagnosis by organizations such as the Endocrine Society or Mayo Clinic.
From a conventional perspective, there is no evidence that the adrenal glands “burn out” due to stress alone.
However, this does not mean the symptoms people experience are not real.
Many practitioners instead describe these patterns as HPA axis dysfunction—a disruption in how the brain and adrenal glands communicate and regulate stress hormones like cortisol.
Addison’s disease (adrenal insufficiency) → measurable hormone deficiency
HPA axis dysfunction → stress-response imbalance
While conventional medicine focuses on diagnosing disease, many patients continue to experience fatigue, poor stress tolerance, and burnout despite “normal” lab results.
This is where an integrative approach becomes essential.
Rather than asking only, “Is there a disease?”, integrative medicine asks:
👉 “Why is the body struggling to maintain balance?”
Patterns often associated with adrenal burnout may reflect:
Chronic nervous system dysregulation
HPA axis imbalance
Blood sugar instability
Inflammation
Gut dysfunction
Long-term effects of stress
For individuals who feel overlooked or stuck, this broader lens provides a path forward—without dismissing their experience.
Addison’s disease is a rare but serious condition where the adrenal glands do not produce enough cortisol (and often aldosterone).
Autoimmune destruction (most common)
Chronic infections
Adrenal damage or bleeding
Genetic conditions
Severe fatigue
Weight loss
Low blood pressure
Salt cravings
Skin darkening (hyperpigmentation)
Nausea or abdominal pain
Dizziness or fainting
In severe cases, an Addisonian crisis can occur and requires emergency medical care.
Addison’s disease requires conventional medical treatment including diagnosis.
Hormone replacement therapy (lifelong)
Ongoing monitoring
While not a replacement, integrative strategies can improve quality of life:
Nutrient support (Vitamin C, B vitamins, magnesium)
Adequate sodium intake
Anti-inflammatory diet
Stress reduction practices
Many individuals experience:
Persistent fatigue
Difficulty waking
Afternoon energy crashes
Brain fog
Sleep disturbances
Anxiety or mood changes
Sugar or salt cravings
Hormonal imbalances
These symptoms are real—but require careful evaluation to rule out other medical conditions.
| Feature | Addison’s Disease | Adrenal Burnout |
|---|---|---|
| Diagnosis | Medical condition | Functional pattern |
| Cortisol | Very low | Dysregulated |
| Cause | Adrenal damage | Chronic stress |
| Treatment | Hormone therapy | Lifestyle + integrative care |
Balanced meals with protein, fats, and fiber help reduce cortisol spikes.
Consistent sleep-wake cycles restore hormonal rhythm.
Breathwork, meditation, and time in nature help shift out of stress mode.
Ashwagandha, rhodiola, and holy basil may support stress resilience.
Excess caffeine can worsen cortisol imbalance.
Look deeper at gut health, inflammation, and chronic stress patterns.
Advanced testing may include:
Cortisol rhythm testing (saliva or urine)
Hormone panels
Nutrient deficiencies
Inflammatory markers
Seek evaluation if you experience:
Severe or worsening fatigue
Fainting or dizziness
Low blood pressure
Unexplained weight loss
Persistent symptoms without answers
Adrenal burnout is a non-medical term used to describe symptoms like fatigue and poor stress tolerance linked to chronic stress and HPA axis dysfunction.
It is not recognized as a medical diagnosis, but the symptoms are real and often related to stress-related hormonal imbalance.
No. Addison’s disease is caused by adrenal gland damage, not chronic stress.
Cortisol can be tested through blood, saliva, or urine testing depending on the clinical approach.
No. It requires lifelong hormone replacement, though lifestyle support can improve well-being.
Vitamin C, magnesium, B vitamins, and adaptogens are commonly used.
It varies, but improvements often occur over weeks to months with consistent support.
Excess caffeine can disrupt cortisol patterns and worsen symptoms.
Whole foods, balanced meals, and stable blood sugar are key.
If symptoms are severe, persistent, or worsening.
Cortisol is not the problem—it is essential for survival. The challenge arises when chronic stress disrupts the body’s natural balance.
For some, this results in clear medical conditions like Addison’s disease. For others, it shows up as ongoing fatigue, burnout, and dysregulation that isn’t always captured through standard testing.
Both experiences are valid—and both deserve attention.
An integrative approach does not replace conventional care—it expands it. It looks deeper at how stress, lifestyle, and physiology interact to influence long-term health.
If you’ve been told everything is “normal” but you don’t feel well, your experience matters—and there are additional paths worth exploring.
Healing is not about quick fixes. It’s about restoring the body’s ability to adapt, recover, and function with resilience over time.
If you’ve been told everything is “normal” but you still feel exhausted, overwhelmed, or out of balance—there may be more to the story.
Our integrative approach looks beyond surface-level symptoms to uncover the underlying factors affecting your energy, stress response, and overall health.
Schedule a personalized consultation today and take the first step toward restoring your resilience, clarity, and vitality.
👉 Book your consultation now
Thanks for investing in your health!
